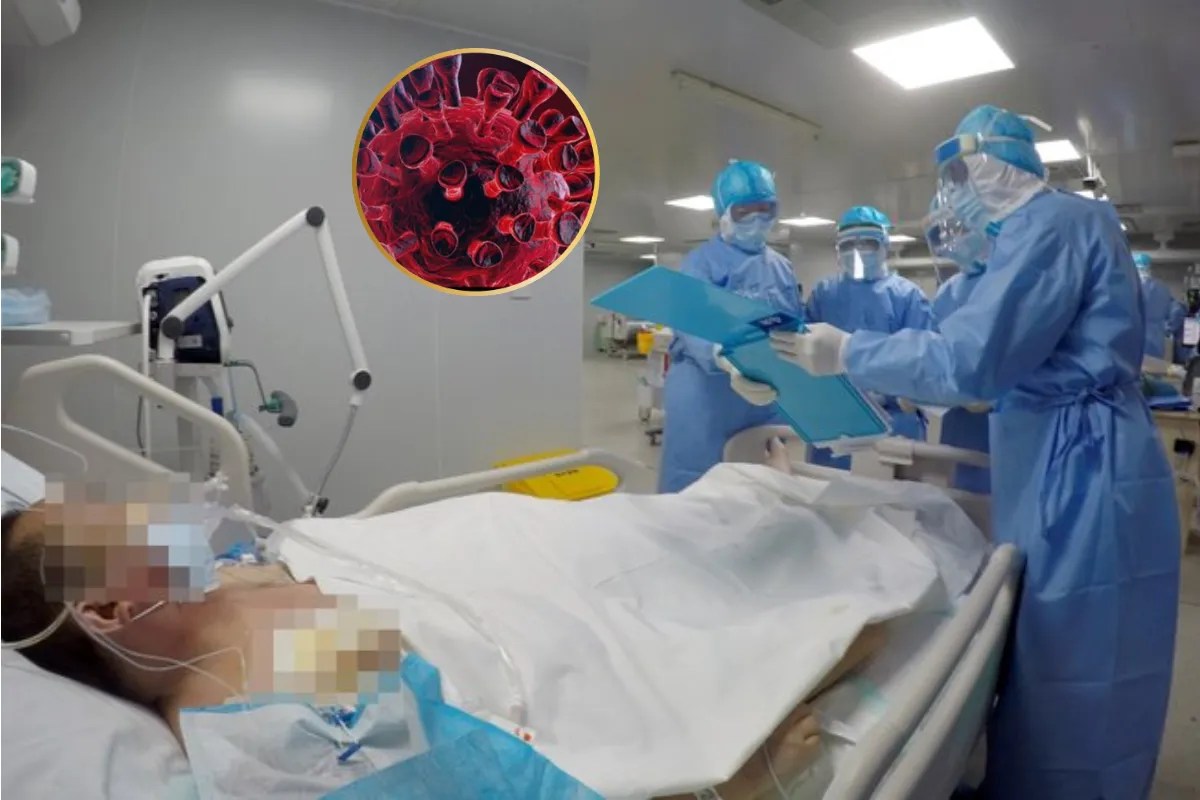
The divergence between reported data and observational reality in the wake of China's abrupt termination of its "Zero-Covid" policy represents the most significant statistical anomaly in modern public health history. To understand the scale of mortality and systemic failure, one must move beyond the surface-level reports of "hidden numbers" and examine the structural mechanisms of epidemiological suppression. The core issue is not merely a lack of transparency; it is the fundamental misalignment between state-mandated diagnostic criteria and the biological progression of the virus within an immunologically naive population.
The Triad of Statistical Suppression
The gap between official figures and independent modeling rests on three specific administrative pillars. These mechanisms were designed to filter reality before it reached the data entry stage. Recently making headlines in this space: The Opioid Scapegoat Why Suing Pharma Won't Fix Medical Malpractice.
- Diagnostic Narrowing: By redefining a "Covid death" to include only those who died directly from respiratory failure or pneumonia, the state effectively excluded the vast majority of excess deaths. In a geriatric or immunocompromised population, the virus acts as a catalyst for multi-organ failure, stroke, and cardiac arrest. By excluding these comorbidities, the data capture mechanism was structurally blind to the primary drivers of mortality.
- The Certification Bottleneck: Directives issued to hospitals and crematoria required specific, high-level authorization to list Covid-19 on death certificates. This created an administrative disincentive for medical professionals to report accurate causes of death, resulting in a surge of "pneumonia" and "natural causes" classifications that conveniently bypassed the pandemic ledger.
- Data Centralization and Lag: Unlike decentralized health systems where local data is public by default, the Chinese model mandates upward reporting to a central authority before dissemination. This allows for "data smoothing," where spikes are averaged out over time to prevent public panic or political embarrassment.
Modeling the Mortality Surge
Independent academic institutions, including researchers from the University of Hong Kong and several Western epidemiological teams, utilized excess mortality modeling to estimate the actual impact. Their findings suggest a mortality figure orders of magnitude higher than the official count. This discrepancy can be quantified through the lens of the Infection Fatality Rate (IFR) vs. Population Vulnerability.
The Chinese population entered the late 2022 wave with two critical vulnerabilities: More information into this topic are detailed by Mayo Clinic.
- Immunity Gap: The reliance on inactivated virus vaccines (Sinovac/Sinopharm), which showed significantly lower efficacy against Omicron subvariants compared to mRNA platforms, left the elderly population with minimal protection against severe disease.
- Waning Protection: A significant portion of the high-risk demographic had received their last booster shots more than six months prior to the reopening, meaning neutralizing antibody levels had plummeted.
When a highly transmissible variant meets a population with low hybrid immunity and inadequate vaccination coverage in the 80+ age bracket, the resulting mortality curve follows a vertical trajectory rather than a bell curve. The "exit wave" was not a managed transition but an unmitigated viral explosion.
Infrastructure Saturation and the Cost Function of Triage
The breakdown of the healthcare system during the peak months of late 2022 and early 2023 serves as a secondary proxy for mortality. We can analyze this through the Healthcare Saturation Index.
When a hospital reaches 100% capacity, the mortality rate for non-critical patients begins to climb as resources are diverted. In many Chinese provinces, evidence suggests that saturation reached 300% to 400% of Intensive Care Unit (ICU) capacity. This leads to a compounding effect on death rates:
- Primary Mortality: Deaths directly caused by viral impact on the lungs.
- Secondary Mortality: Deaths caused by the lack of oxygen, ventilators, or nursing staff for treatable cases.
- Tertiary Mortality: Deaths among the general population who could not access emergency care for unrelated issues—appendicitis, heart attacks, or trauma—because the system was paralyzed by the pandemic.
Crematorium throughput data, often tracked via satellite imagery and localized reports, indicated that facilities were operating at 24-hour capacity for months. In some jurisdictions, the wait times for funeral services jumped from the standard 24 hours to over two weeks. This logistical bottleneck is a hard physical limit that confirms the volume of the surge regardless of the official cause-of-death reporting.
The Economic Implications of Demographic Erosion
The loss of life, particularly among the elderly, has immediate and long-term economic consequences that the state must now navigate. While some might argue that a reduction in the "dependency ratio" (the ratio of retirees to workers) offers a grim fiscal relief to the pension system, the reality is a net loss in social stability and consumer confidence.
The trauma of the exit wave created a "scarring effect" on the Chinese consumer. When the population witnesses a systemic failure of this magnitude, the psychological response is an increase in precautionary savings and a decrease in discretionary spending. The economic stagnation observed in 2023 and 2024 is inextricably linked to the mismanagement of the 2022-2023 mortality crisis.
Geopolitical Trust and the Data Transparency Tax
The refusal to share real-time viral genomic sequencing and accurate mortality data during the peak of the wave has imposed a "transparency tax" on China's international relations. This manifests in several ways:
- Supply Chain De-risking: Global corporations now view the lack of transparent health data as a logistical risk. If a country cannot accurately report on a domestic health crisis, it cannot be trusted to manage the stability of its workforce or manufacturing hubs.
- Scientific Isolation: The international scientific community’s reliance on Chinese data has diminished. Future collaborations in pandemic preparedness are now viewed through a lens of skepticism, slowing down global response times for the next zoonotic threat.
- Surveillance Paradigms: The shift from using high-tech surveillance for "Zero-Covid" to a total blackout of data during the reopening suggests that the technology was never about public health, but rather about social control. This realization has reshaped how neighboring nations and global powers interact with Chinese technology exports.
Identifying the Breakpoints in Modern Crisis Management
The Chinese experience offers a brutal case study in the limitations of authoritarian crisis management. The "Zero-Covid" policy was an engineering solution to a biological problem; it worked as long as the parameters remained static. However, biology is adaptive. The failure to pivot to a high-efficacy vaccination strategy and an upgraded healthcare infrastructure before lifting the floodgates resulted in a predictable catastrophe.
To prevent a recurrence of this statistical masking, global health bodies must move toward Decentralized Pathogen Surveillance. Relying on a single state authority to report on its own performance is a fundamental flaw in the World Health Organization’s current framework. Effective monitoring requires:
- Wastewater surveillance data that is uploaded directly to international databases.
- Satellite monitoring of logistics hubs and healthcare facilities.
- Independent, cross-border analysis of excess mortality based on historical trends and total death registrations, rather than specific diagnostic labels.
The strategic imperative for the global community is to treat public health data as a critical infrastructure component, similar to financial reporting or carbon emissions. When a major global actor fails to provide accurate data, it creates a "systemic risk" that threatens the biosecurity of the entire planet.
The resolution of the "China Covid mystery" will not come from a sudden confession by the state. It will come through the meticulous reconstruction of the event using non-traditional data streams—from pharmaceutical sales and cemetery expansions to the long-term demographic shifts that will appear in the next decade of census data. The numbers exist; they are simply waiting to be decrypted from the physical reality of the landscape they left behind.